According to U.S. Center for Disease Control and Prevention (CDC) estimates, around 2 million people are infected with resistant bacteria each year, killing 23,000 overall.
Harmful bacteria that can’t be treated with standard bacterial fighting drugs – antibiotics – are known as drug-resistant. Because the drugs that would normally kill them have no effect, they’re often referred to as superbugs.
Superbugs are a current concern — not a threat of future, warned the World Health Organization
“The world is headed for a post-antibiotic era, in which common infections and minor injuries which have been treatable for decades can once again kill,” said Dr. Keiji Fukuda, WHO’s Assistant Director-General for Health Security. Unless the world acts now, “the implications will be devastating.”
This means that conditions as routine as a sinus infection, bronchitis, ear pain, strep throat — things that normally can be treated with antibiotics — could become deadly.

CDC.gov
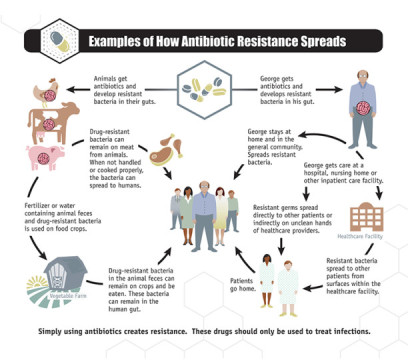
Overuse of antibiotics is considered one of the big reasons that bacteria develops resistance against drugs. The CDC explains:
Every time a person takes antibiotics, sensitive bacteria (bacteria that antibiotics can still attack) are killed, but resistant bacteria are left to grow and multiply. This is how repeated use of antibiotics can increase the number of drug-resistant bacteria.
Antibiotics are not effective against viral infections like the common cold, flu, most sore throats, bronchitis, and many sinus and ear infections. [But] widespread use of antibiotics for these illnesses is an example of how overuse of antibiotics can promote the spread of antibiotic resistance.
While it can happen anywhere, hospitals and nursing homes are more prone to heightened infection rates and deaths due to superbugs. Close-knit communities are also at a higher risk, according to a 2013 CDC report.
CDC.gov
In 2013, the CDC released a report on the top 18 drug-resistant threats, classifying them for the first time by severity: urgent, serious, and concerning. One of the urgent superbug threats is Clostridium Difficile (CDIFF), one of the causes of sepsis. Sepsis infects 1 million hospital patients in the U.S. every year; the CDC estimates half will die from the infection.
The complete list and more details about these superbugs can be found here.

Michael Mortensen via Flickr
In order to prevent an increase in superbugs, the National Institute of Health suggests “taking antibiotics properly and only when needed.” Patients should not insist on a an antibiotic if their health care provider advises otherwise, they added. In March 2015, the Obama administration released a five-year plan to fight superbugs.
The CDC suggests these steps to prevent the formation and spread of superbugs:
- Preventing infections/spread of resistance.
- Tracking and early reporting new cases of drug-resistant bacteria.
- Improving antibiotic stewardship preventing unnecessary use of antibiotics.
- Developing new drugs and tests that could help track and slow down the growth and development of these superbugs.
 CGTN America
CGTN America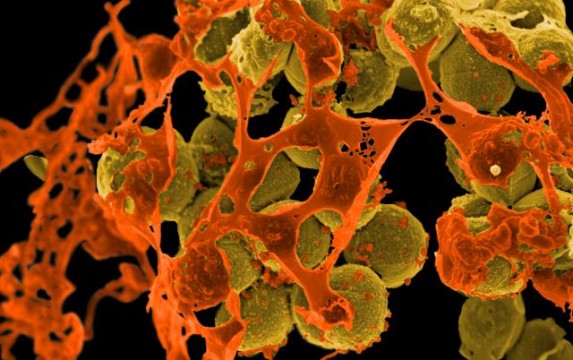 Methicillin-Resistant Staphylococcus aureus (MRSA) Bacteria ( Photo: NIAID via Flickr)
Methicillin-Resistant Staphylococcus aureus (MRSA) Bacteria ( Photo: NIAID via Flickr)
